Mac’s father, Tyler, overdosed on pure fentanyl. His family believes he thought it was heroin. Mac says he wants to speak out and share his story “because it’s a really big problem in the world and a lot of other people are suffering because of it, because of drugs.”
Tyler was one of 978 overdose deaths in B.C. alone in 2016, which was the worst year for drug deaths in the province’s history. But preliminary data for 2017 shows there were 1,013 overdose deaths at the end of August, already surpassing last years total. If the current rate continues, B.C. could see more than 1,500 deaths by the year’s end.

Trevor Jang
It’s unknown how many children like Mac have lost a parent during the opioid crisis — according to the B.C. Coroners Service this is not a statistic that is tracked. But the crisis has claimed the lives of thousands of people across Canada over the past two years and the kids left behind are at high risk of developing substance abuse issues themselves. Now, some families are struggling to navigate the mental health system, desperate to prevent children of addicts from repeating their parent’s mistakes.
“My grandchildren are at risk for mental health and drug misuse. Even though they both swear, because of what happened to their dad, they’ll never use,” says Helen Jennens, Tyler’s mother and Mac’s grandmother. Jennens’ eldest son, Rian, died of a prescription drug overdose in 2011. Since losing both of her sons to overdose in the span of five years, Jennens has become an outspoken advocate for improved addiction services. She wants to make sure Mac and his younger sister Talay can move forward and overcome their trauma.
“They need support from family. They need support at school. They need support from the medical community. They need counselling. There’s a lot going on that needs to be addressed as they get older,” Jennens says.
Waiting months for help
Finding that help hasn’t been an easy process, nor a fast one. Jennens says it took six months to get a mental health assessment for Mac and Talay, and then another four months before their first counselling appointment.
Looking across the country, this is not an uncommon story. As Discourse Media previously reported, according to the Mental Health Commission of Canada an estimated 1.2 million children and youth in Canada are affected by mental illness, yet less than 20 per cent will receive appropriate treatment. In Ontario, nearly 12,000 kids are waiting for long-term psychotherapy, with some children and youth in need of urgent care waiting up to 18 months for mental health support.
“A lot of services for mental health and addiction are still not publicly funded or publicly available,” says Amanda Butler, SFU researcher and co-author of the study Toward Quality Mental Health Services in Canada. “For those who can’t afford private services, the reality is just that the public services are insufficient to meet the demand of the people who need it.”
“There needs to be more money but it also just needs to be spent more wisely,”
Amanada Butler, SFU researcher. The 2017 study of five provinces found that for about 40-50 per cent of affected children, their first contact with the mental health system is the emergency department. “There’s a good indication that we’re not doing enough in schools to recognize mental illness and plan for early intervention,” Butler says, though she can’t specifically speak on the impact of the opioid epidemic on Canadian youth left behind due to a lack of data on the subject.
So, to find out if there are any services specifically created for children who lose a parent to an overdose, Discourse Media contacted every province and territory in the country. Five provinces and two territories responded, each pointing to various forms of publicly-funded counselling services. None of the provinces or territories had information on services specifically designed for children affected by the opioid crisis.
What we do know is that access to psychologists can take time. The Psychological Association of Canada (PAC), says that their members tell them “wait times to see a psychologist in the school system can range from months to a year or more — this is because of the limited amount of psychological resource in schools.”
Most of the 18,000 registered psychologists in the country work in the private sector. “Some psychologists work in the public sector (schools, hospitals, or publicly-funded clinics), given budget pressures and working conditions in public institutions, more and more psychologists work in the private sector,” wrote a PAC representative in an email.
The number one barrier to mental health services is a lack of public funding, according to the Mental Health Commission of Canada. In 2015, Canada spent $15.8 billion on mental health care, representing 7.2 per cent of the country’s total health spending. The Mental Health Strategy for Canada recommends raising the annual percentage to nine per cent by 2022.
But Butler says money is only part of the story. “There needs to be more money but it also just needs to be spent more wisely. We can’t make decisions about how to more effectively spend until we actually can do proper research and follow the data to see what’s working for people,” she explains.
“We actually don’t have the ability in Canada right now even to measure the status quo. We don’t know how well we’re doing and whether the services we are providing are actually leading to meaningful change,” says Butler.
Preventing the cycle
Jennens is still looking for answers from Canada’s mental health system. Her search for help started in 1987, when her eldest son Rian began struggling with mental health and substance use issues. “There wasn’t a lot. Unless you were cutting yourself or talking about committing suicide, or hurting other people, there just wasn’t anything available,” she recalls.
Her other son Tyler had been battling an opioid addiction since 2010. He ruptured his achilles playing football and was prescribed oxycontin, explains Jennens. By the time his prescription ran out, he was hooked, she says. Jennens believes Tyler’s addiction escalated to heroin a year later after his older brother’s overdose.
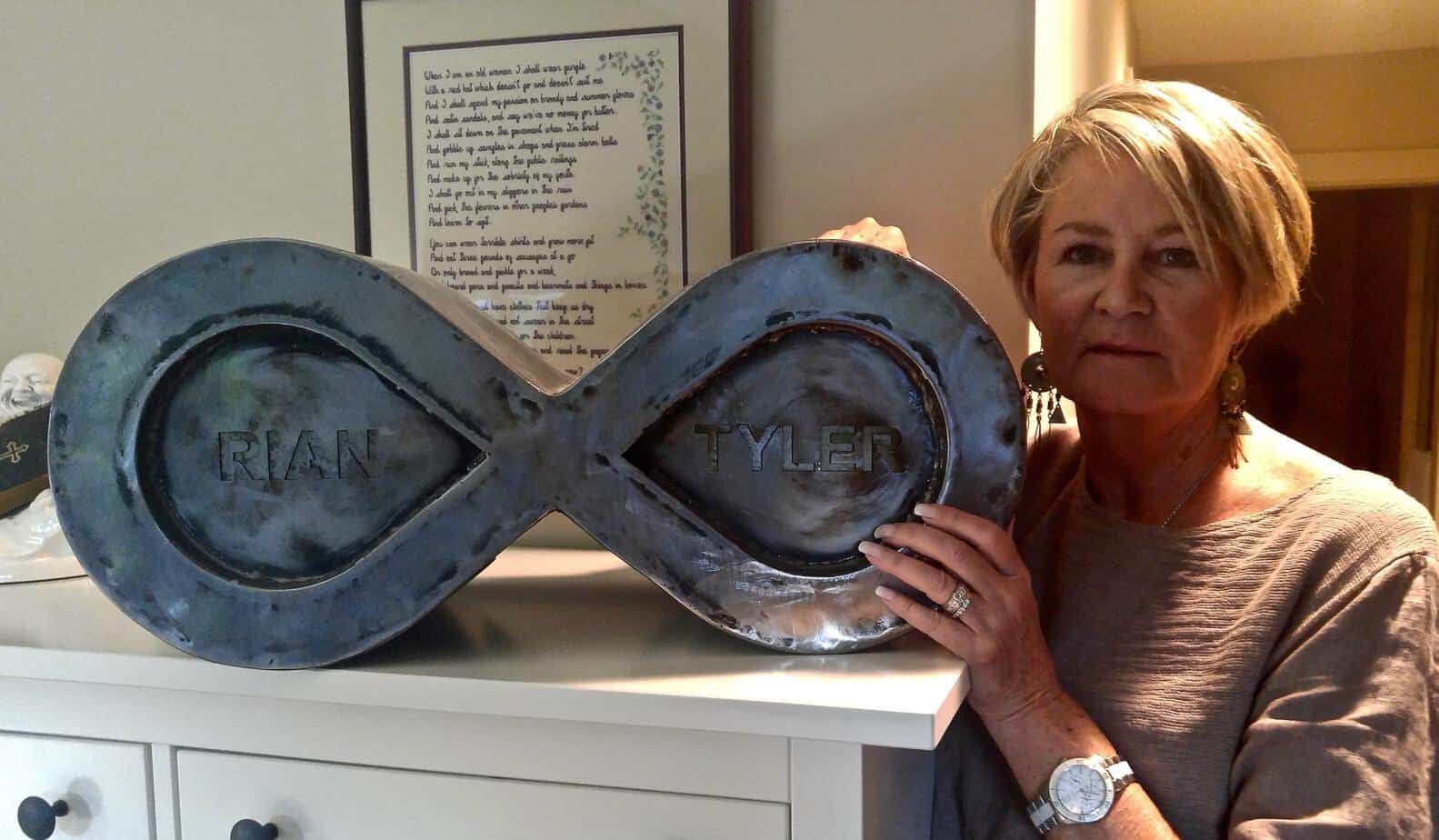
Trevor Jang
Jennens struggled to find Rian help as a teenager. Similarly, she struggled to get Tyler help as an adult. “We could get him drug-free for eight or nine or 10 months, but because what was going on in his head was so awful, and part of that was the destruction of his life through the drug abuse, he would end up relapsing. He couldn’t cope with what was going on in his head.”
In that time, Mac watched his father turn from an outgoing and charismatic hero, a man who once saved a drowning boater at sea, into a man who would buy heroin while babysitting his kids. “He was still a really nice man, but you could tell he wasn’t happy any more,” Mac recalls. “He was still always nice to his children and everything, but the drugs really changed him.”
Now, Jennens wants to make sure that her grandchildren don’t repeat these mistakes. She’s not alone either. Across the country, it’s estimated that 8.9 million Canadians will suffer from a mental illness or addiction by 2041, up from 6.7 million today. And 70 per cent of those mental illnesses will begin during adolescence.
“If we can catch them at age 14 with some of their issues, we might not be burying them at age 20 from an overdose,” she says.
Fighting for help
Following Tyler’s death, Jennens joined Moms Stop the Harm, a network of Canadian families who have lost a loved one to drugs. The group fights the stigma associated with addiction. Jennens also joined a collaborative known as Child and Youth Mental Health and Substance Use, which fought for years to bring a youth-focused health services hub to Kelowna and succeeded.
Kelowna now has Foundry, a hub that brings together 25 partner organizations under one roof in an attempt to be a “one stop shop” for all the mental health needs of young people aged 12-24. The centre is one of five pilot locations throughout the province receiving $500,000 annually from the B.C. government to operate, with five more expected to open in the near future.
“The grand vision for this is that all organized communities across British Columbia would have a Foundry so that young people know the place to go when they need help,” says Mike Gawliuk, Director of Service Delivery and Program Innovation with the Canadian Mental Health Association Kelowna, the lead agency tasked with operating Foundry Kelowna. Gawliuk says more than 100 young people have received help since they opened in August of 2017, and he expects the centre to support between 1250 and 2000 youth on an annual basis.
Jennens hopes this means there is finally a place for her grandchildren to turn to for help. She shares her family’s story in an effort to fight the stigma associated with addiction and has encouraged Mac to do the same. His advice for people struggling with a drug addiction: “I think they should get care. They should go to a counsellor and get all the support that they need so they can continue on with a nice life.” [end]
This story follows an in-depth feature by reporter Trevor Jang about his family’s personal experience with addiction, it can be viewed here. This story was edited by Lindsay Sample. Discourse’s executive editor is Rachel Nixon.
This story was updated on October 12 to include new numbers from the B.C. Coroner’s Service on illicit drug overdose deaths for 2017.
[cta]
Have you or a family member had to wait to access treatment? Or, did you receive treatment quickly? We want to hear from you. Email trevor@discoursemedia.org.
[/cta]
Resources: We want to take this opportunity to share some of the resources available for people dealing with mental health and addictions issues. If you are in crisis and in need of immediate help please call 9-1-1. Young people under the age of 20 can get anonymous and confidential counselling by calling the Kids Help Phone for free at 1-800-668-6868 or using the online chat function on their website. For anyone having feelings of distress or despair, including thoughts of suicide, you can call 1 800 SUICIDE (784-2433) for free, non-judgemental support.
Residents of B.C. can call 8-1-1, a free-of-charge provincial health information and advice phone line available for non-emergency health information. A detailed list of provincial and territorial addictions treatment helplines can be found here.
What did you think of this story?
Your feedback after we publish a story helps ensure we're always improving our reporting to better serve you
Author
Trevor Jang is an award-winning journalist and writer with a passion for Indigenous issues. He was a recipient of the 2016 CBC Indigenous Fellowship through the Canadian Journalism Foundation and a finalist for the 2016 British Columbia Association of Broadcasters Excellence in News Reporting award. Trevor spent two years hosting a radio show on Canada’s First Nations Radio (CFNR) Network in northern B.C. which focused on First Nations culture, music and issues. He is a mix of Chinese-Canadian and Wet’suwet’en descent.
Related Articles
Legal heroin needed to save lives and money, experts say
Canada's health minister announced support for prescription heroin, but Ottawa still won't consider decriminalizing hard drugs — a step that experts say would further reduce…
Q&A: Ojibway artist on what it’s like to visualize addiction and trauma
Joshua Mangeshig Pawis-Steckley, the illustrator for Discourse's #KidsofAddiction series, talks his art and inspiration.
Kids of addiction
What my father's overdose death taught me.